As part of interprofessional teams, chiropractors offer their expertise to help vulnerable patients with low back pain in six of seven primary care sites across Ontario.
The Challenge:
- Low back pain is the leading cause of disability worldwide, according to estimates from the 2015 Global Burden of Disease Study – and Ontario is no exception.1
- Patients with spine, muscle and joint issues often visit multiple care providers, including primary care physicians, specialists and emergency departments seeking help – adding up to about $2.4 billion in annual costs to Ontario’s health care system.2
- Back pain has been reported in more than half of people who regularly use opioids.3
- A number of Ontarians with low back pain and other health conditions have no extended health benefits and negligible disposable income to access the care they need.
The Primary Care Low Back Pain program offers vulnerable patients with low back pain a way to access the care they need.
Building on Research and Results
Chiropractors provide spinal manipulation therapy, which The American College of Physicians clinical practice guideline recommends as an effective first-choice treatment for low back pain.4
How the Primary Care Low Back Pain (PCLBP) Program Works
The government-funded PCLBP program supports interprofessional primary care teams, including family health teams, nurse practitioner-led clinics and community health centres. These interprofessional primary care teams were formed to deliver efficient, coordinated and integrated care to patients with low back pain.
To achieve this goal, these teams include spine, muscle and joint experts, such as chiropractors, physiotherapists, kinesiologists, occupational therapists and registered massage therapists, who work directly with patients.
When a physician or nurse practitioner refers a patient to the PCLBP program, the patient meets with one of these experts on the interprofessional team, such as a chiropractor, who:
- Assesses their low back pain
- Develops an evidence-based care plan for them
- Refers them to one or several team members for education and regular treatment, such as spinal manipulation therapy and a therapeutic exercise program
In 2015, the Ontario Ministry of Health and Long-term Care launched Primary Care Low Back Pain pilots at the following seven sites across Ontario:
- TAIBU Community Health Centre (Scarborough, ON)
- Centre de santé communautaire de l’Estrie and Glengarry NPLC (Cornwall and Alexandria, ON)
- Mount Forest, East Wellington and Minto-Mapleton Family Health Team (Mount Forest, East Wellington and Minto-Mapleton, ON)
- Couchiching Family Health Team (Orillia, ON)
- Belleville Nurse Practitioner-Led Clinic (Belleville, ON)
- Essex Court NPLC & City Centre Health Care (Windsor, ON)
- Shkagamik-Kwe Health Centre (Sudbury, ON)
After their completion, the province transitioned the PCLBP pilots into programs at the seven sites and provides ongoing, base funding to sustain them.
How the PCLBP Program Helps Ontarians
PCLBP program patients often have other health conditions, such as diabetes, addictions or hypertension, as well as a low income and no extended health care benefits. Without this program, many of these patients would be unable to access low back pain care.
Overall, the Ontario government-funded PCLBP program is designed to:
- Improve these patients’ experience and their results
- Reduce unnecessary diagnostic imaging and MRI tests
- Reduce unnecessary referrals to specialists
How the PCLBP Program Can Help You
Eligibility Requirements
You may be eligible for the PCLBP Program if you:
- Have low back pain and/or related symptoms
- Are a patient of one of the seven interprofessional primary care teams the program is offered in, or live near one of the seven locations and receive a referral from your physician or nurse practitioner
This program is free of charge, if you do not have extended health care coverage.
If you have low back pain and/or related symptoms and meet the PCLBP program’s eligibility requirements:
- Make an appointment with your family physician or nurse practitioner to ask about a referral to the PCLBP program.
- If you’re referred to a PCLBP program site, you’ll meet with a member of the site’s interprofessional team within about four weeks from the referral date.
- A member of the site’s interprofessional team will assess your condition, provide you with useful information about it and develop an evidence-based care plan for you. They will also refer you to one or several team members for education and treatment.
Chiropractors’ Impact on the Primary Care Low Back Pain Program
Chiropractors are providing care to patients with low back pain at six of the seven PCLBP program sites across Ontario.
Outcomes:
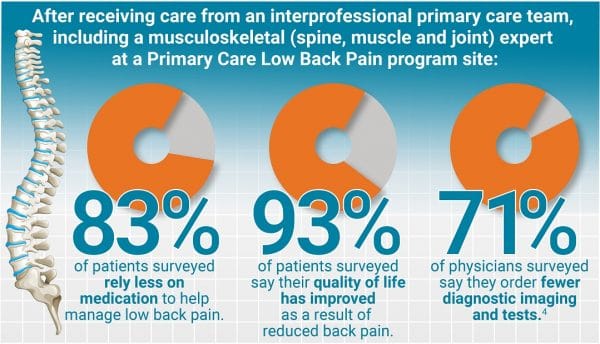
Of the patients surveyed at one PCBP program site, evaluation results found:5
- 94 per cent of patients were satisfied or extremely satisfied with assessment and treatment received.
- 93 per cent of patients agreed that their quality of life has improved.
- 87 per cent of patients agreed the program gave them access to low back pain treatment they otherwise wouldn’t be able to access.
- 83 per cent of patients agreed they now rely less on medication to help manage low back pain.
In addition, these patients have also significantly reduced their:
- Use of Emergency Rooms
- Referrals for diagnostic imaging
What PCLBP Pilot/Program Patients Say …
“Because my chiropractor is in contact with my nurse (practitioner) whom I see on a regular basis… They’re looking at me as a whole piece, not just fixing (a part of me). They’re trying to see what they can do to help me be better as a whole.”
“Thank you (to my chiropractor) for helping me with the back pain I have suffered over eleven years… I was taking 6 Percocet per day, along with 6 Tylenol #3. After only a few adjustments I started to feel so much better. I have (now) eliminated the Percocet and Tylenol #3 and now have no pain.”
What Health Care Professionals Say …
“The simple access piece … this is a free service so I think historically perhaps people were suffering in silence … now you offer the service and people have an opportunity to access that service with no out of pocket expenses, so they’re no longer suffering in silence”
“I’m impressed with the effects of the PCLBP project. My clients report much improvement – not only with pain control but also energy and function. They require less medication and have huge improvements in quality of life.”
In the News:
- Chiropractors team up with community health centres to care for those in need, The Globe and Mail