How Will Chiropractors Address the Opioid Crisis?
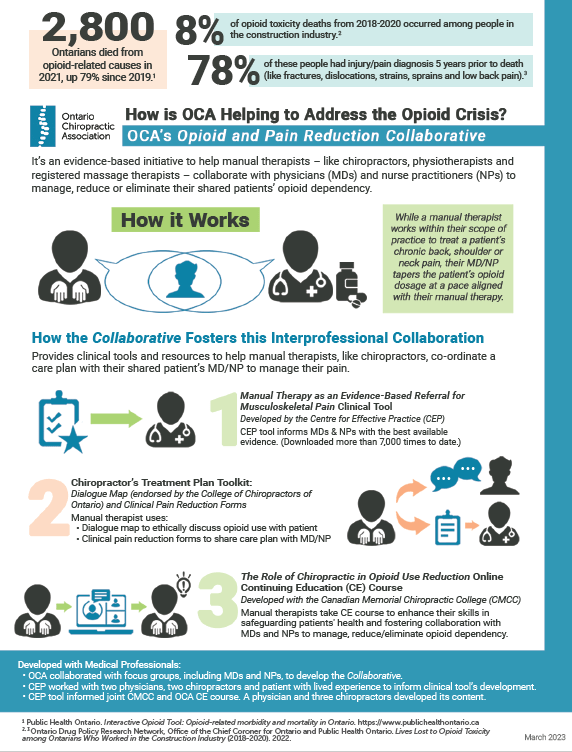
In collaboration with medical professionals, we developed the Opioid and Pain Reduction Collaborative (the Collaborative). It’s designed to help chiropractors manage their patient’s long-term (chronic) back, shoulder and neck pain while collaborating with their medical doctor/nurse practitioner to manage or reduce their opioid dependency.
Research results demonstrate that treatments chiropractors provide can effectively help patients with chronic back, neck and/or shoulder pain. They can also do so without medication and reduce patients’ reliance on opioids.
Unfortunately, evidence-based recommendations considering manual therapy for pain management, and how to introduce and oversee this care, are not widespread.
To bridge these gaps, we consulted with an interprofessional advisory panel and hired the Centre for Effective Practice (CEP) to produce a clinical, knowledge translation tool.
-
This Manual Therapy as an Evidence-Based Referral for Musculoskeletal Pain Clinical tool is for medical doctors and nurse practitioners.
-
The advisory panel included Dr. Janice Harvey MD, CCFP(SEM), FCFP DIP. SPORT MED, Dr. David Dos Santos, B.Sc., D.C., FCCPOR(C), FCCO(C), Dr. Erica Weinberg, BSc, MSc, MPhil, MD, Dr. Lindsey Rebeiro, BScH, DC and Lynn K. Cooper, BES as a patient with lived experience.
To support chiropractors, we produced the Chiropractor’s Pain Management Toolkit (for chiropractors to explore opioid management with a patient). A key part of the Chiropractor Pain Management Toolkit is the Chiropractor Dialogue Map. The CCO unanimously endorsed this dialogue map, making it clear that chiropractors using this tool are within their scope of practice.
The Collaborative equips health care professionals with the information they need to work together, helping their patients manage their back, shoulder and neck pain while managing or reducing their dependence on opioids.
How the OCA Opioid and Pain Reduction Collaborative Tools Address the Opioid Crisis
Part 1 – Manual Therapy as an Evidence-Based Referral for Musculoskeletal Pain Clinical Tool
We hired the CEP to develop this evidence-based clinical tool to help medical doctors (MD)s and nurse practitioners (NP)s navigate manual therapy.
This tool gives MDs and NPs the best available evidence they need to refer patients with back, neck and shoulder pain to a manual therapist and co-ordinate a plan of care with them. With their pain managed through these medication-free therapies, patients can use and depend less on opioids to manage their pain.
In addition, the Centre for Addiction and Mental Health (CAMH) included this tool in its Opioid De-implementation Pathway for medical doctors.
Part 2 – Chiropractor’s Pain Management Toolkit
We developed this toolkit to help chiropractors best navigate communication with patients who want help managing their opioid usage, as well as their medical doctors/nurse practitioners. It works by making the communication pathways easier for all health care professionals in the circle of care. The Pain Reduction Toolkit includes a Chiropractor Dialogue Map and three, fillable pain reduction forms to support collaborative care.
Check the following podcast series on addressing the opioid crisis to learn more about this toolkit and how to best use it:
Part 1 – Breaking the Ice on Opioid Dependency
Part 2 – Building Rapport with a Prescribing Health Professional
We partnered with the Canadian Memorial Chiropractic College (CMCC), an international leader in academic scholarship and training, to develop and launch The Role of Chiropractic in Opioid Use Reduction, a practical continuing education (CE) course for chiropractors in early 2022. It empowers chiropractors to start a potentially life-changing conversation with patients and their medical doctors or nurse practitioners to collaboratively manage, reduce or eliminate their patients’ opioid dependencies.
Using Research and Results to Address the Opioid Crisis
Treatments that chiropractors provide, such as spinal manipulation and therapeutic exercise programs, have effectively helped patients with chronic back, neck or shoulder pain, without medication and can reduce their reliance on opioids.
For example:
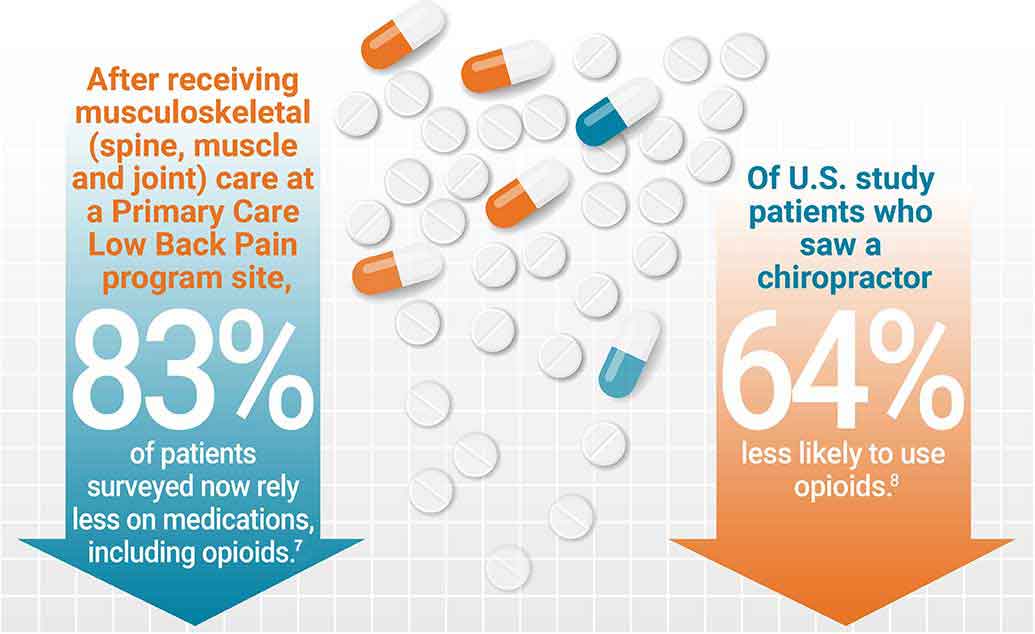
- 83 per cent of patients surveyed at one of Ontario’s Primary Care Low Back Pain (PCLBP) sites now rely less on medication, including opioids, to help manage their low back pain. This survey was conducted after patients received care from a musculoskeletal expert, such as a chiropractor.7
- A 2019 U.S. study found that 64 per cent of patients who saw a chiropractor were less likely to use opioids.8
Subsequently, many medical authorities recommend health care professionals, such as medical doctors (MD)s and nurse practitioners (NP)s, consider pain management therapies without medication, including those chiropractors provide, before opioids:
- 2017 Canadian Guideline for Opioid Therapy and Chronic Non-Cancer Pain recommends coordinated multidisciplinary collaborations between medical doctors and other health professionals, such as chiropractors.9
- The American College of Physicians Low Back Pain Systemic Review demonstrated that exercise is effective for reducing long-term (chronic) low back pain and spinal manipulation provided better short-term pain relief than other active interventions.10
- Health Quality Ontario suggests that making better use of non-medical treatments to manage both short-term (acute) and long-term (chronic) pain will reduce the number of people who end up using opioids for the long term. It will also reduce the number of prescription opioids that people use in harmful ways.11
Chiropractic care can help address the opioid crisis because it’s effective for treating a patient’s chronic back, neck, shoulder pain. When this care treats their pain, chiropractors can collaborate with patients and their MDs/NPs to reduce or manage opioid dependency.
How the OCA Opioid and Pain Reduction Collaborative Will Help Ontarians
Over time, the Collaborative is expected to contribute to helping:
• Reduce the number of Ontarians who depend on opioids to manage their chronic back, shoulder or neck pain
• Decrease the number of opioid-related fatalities in Ontario and across Canada
• Increase the effectiveness of patient-centred care
For a broader perspective on how the Collaborative will help address the opioid crisis, particularly given its tragic rise during the COVID-19 pandemic, please check our CEO blog post: Addressing the Opioid Crisis with Interprofessional Collaboration.
Chiropractors’ Impact
As the OCA Opioid and Pain Reduction Collaborative is implemented, chiropractors will collaborate with medical doctors and nurse practitioners to help patients learn how to manage their chronic back, shoulder or neck pain, without depending on opioids.
Why We Need to Address the Opioid Crisis:
- In Ontario, there were close to 2,000 deaths related to opioid use in 2019 alone. 1
- Back pain has been reported in more than half of all regular opioid users.2 And, is one of the most common diagnoses emergency and family physicians cite for prescribing opioids.3
- A study at the Pain Management Centre at Hamilton General Hospital among patients prescribed long-term opioid therapy for chronic, non-cancer pain found 64.8 per cent of patients received this therapy for chronic low back pain.4
And even though many patients are prescribed opioids for pain, a 2016 systematic review and meta-analysis found that opioid medications provide only modest, short-term pain relief for people with chronic (long-term) back pain.5 Furthermore, in 2020, a systematic review and meta-analysis concluded that avoiding prescribing opioids for acute spine, muscle and joint injuries to patients with past or current substance use disorder, restricting duration to seven days or less and using lower prescribed doses when prescribed, are potentially important goals to reduce rates of persistent opioid use.6
What patients, who are former opioid users, say about chiropractic treatment…
“Thank you [to my chiropractor] for helping me with the back pain I have suffered over eleven years… taking 6 Percocet per day, along with 6 Tylenol #3… I have (now) eliminated the Percocet and Tylenol #3 and now have no pain.”
“I got hit back in 2005 on my bike. I was taking percs [Percocet], buying them off the street, I was taking anything I can get to stop the pain. Now [after chiropractic care] I’m right off the percs!”
To learn more about the OCA Opioid and Pain Reduction Collaborative, visit:
In the News:
“If a patient’s pain is well controlled by the treatment they received from a chiropractor, they may subsequently need less pain medications or even none at all.” Dr. Kelsey Corcoran, Yale School of Medicine
“Currently opioids are prescribed for pain management but we’ve recognized there are some potential issues with that, and so considering non-pharmacological alternatives are a great addition to the primary care physician’s tool box. Referral to a chiropractor will actually help potentially avoid the necessity to prescribe opioids.” Steven Passmore, University of Manitoba
“A lot of people that suffer from opioid addictions was initially from pain. What we offer is non-pharmaceutical base care, so we can help them not get to the point where they have chronic pain and need stronger medication to help.” Dr. David Peeace, chiropractor